Your Cart is Empty
What To Expect From Transdermal Verapamil 15% Gel
What To Expect From Transdermal Verapamil 15% Gel
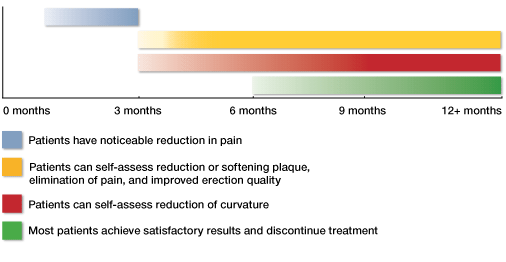
Treatment Timeline
It is important to understand that there are no "quick fix" treatments for Peyronie's disease. This is because remodeling tissue is a slow process. Patients should expect to use Transdermal Verapamil 15 Percent Gel for a minimum of six months and should realistically expect to use the medication for 9 to 12 months to complete their treatment. Patients who are experiencing painful erections typically see this as the first symptom to be resolved, usually within 90 days. Also by 90 days, patients typically can feel a reduction or softening of the plaque. Once the plaque has started to remodel, the curvature and deformities begin to decrease. Transdermal Verapamil 15 Percent Gel is not a life long treatment and it is not necessary to use the medication periodically as a maintenance or preventative treatment.
What Happens If I Am Not Getting Better?

As with any medication, Transdermal Verapamil 15% Gel will not help everyone; however, PDLabs wants to make every effort to maximize the results patients receive. Patients that are not responding tend to fall into one of two categories. First are patients that do not improve at all and patients that have responded but seem to have reached a plateau and no longer improving. All patients are started on a regimen of one dose twice a day since this is effective for the majority of patients. If you are not responding at this dose, a PDLabs pharmacist will contact your doctor to discuss alternative doses that have proven effective in other patients that might be appropriate for you.
Side Effects
The most common side effect reported with Transdermal Verapamil 15% Gel, affecting 3-5% of patients, is varying degrees of skin irritation. Some patients using the medication for the first time may experience mild itching/irritation during the first few days of treatment. This is normal and usually resolves within 3-4 days. Other patients may experience more severe skin irritation, including itching, burning, redness, or swelling. More persistent or severe irritation can usually be treated with over-the-counter topical corticosteroids such as 1% hydrocortosone or with Aquaphor® to treat the dryness of the affected skin. Based on the individual symptoms, PDLabs will work with the patient and prescribing physician to determine the best course of treatment to resolve irritation.
Get The Most From Transdermal Verapamil 15% Gel
Using Transdermal Verapamil 15% Gel Correctly

To get the most from Transdermal Verapamil 15% Gel it is critical that you use it correctly. In order to maintain a steady level of the collagenase enzyme that is responsible for remodeling the plaque, the medication must be applied very consistently. Patients that skip doses or days of application, typically see very slow or no improvement in their condition. Transdermal Verapamil 15% Gel should be applied twice a day, approximately 12 hours apart. Remember to allow a few days to get your prescription refilled so that you do not run out of medication.
Keeping Your Doctors Appointments
It is important to keep your appointments with your doctor. Since improvements in your condition occur over time with Transdermal Verapamil 15% Gel, it is often difficult to objectively determine how much your condition has improved. Your doctor will keep notes that can be objectively compared at each exam. You will also want to print out a copy of the symptom checklist for each visit so that you can talk to your doctor about the progress you are making. This will also be helpful in determining if a change in your regimen is necessary to obtain the best possible results.
Advantages of Transdermal Verapamil 15% Gel
The most important advantage to Transdermal Verapamil 15% Gel is that it is non-invasive. This eliminates the possibility of worsening your condition as often happens with invasive treatments.
Due to the density of the plaque, injection therapies such as verapamil, corticosteroid, and interferon injections are unable to effectively dispense enough medication to the entire primary plaque in one injection. Therefore, multiple injections must be made which may cause additional trauma to the surrounding tissue and worsen the condition. Additionally, since injection therapy only pinpoints the palpable plaque, any non-palpable plaque in the penile shaft is left untreated, resulting in a less effective treatment.
Iontophoresis (electromotive) treatment, like injections, only pinpoints the palpable plaque. Any non-palpable plaque of the penile shaft is left untreated, resulting in a less effective treatment. This treatment is typically not recommended in more severe cases.
Surgery poses risk of additional trauma to penile tissue and is only able to remove the primary plaque; any other fibrosis in the shaft is left untreated. Surgery can have negative post-operative side effects, including significant decrease in penile length and/or girth, erectile dysfuntion, or the return of the condition.
Oral medications (vitamin E, colchicine, para-amino benzoate (Potaba®), etc.) are unable to sufficiently concentrate in the plaque due to systemic absorption and metabolization in the first pass through the liver.
